Oxygen keeps you alive. Every breath, every heartbeat, every thought you’ve ever had depended on it. So it seems almost impossible that the same gas could hurt you. But it can. And it does.
When a patient uses too much oxygen, the body doesn’t celebrate. It pushes back. Hard.
The Paradox of Oxygen Therapy
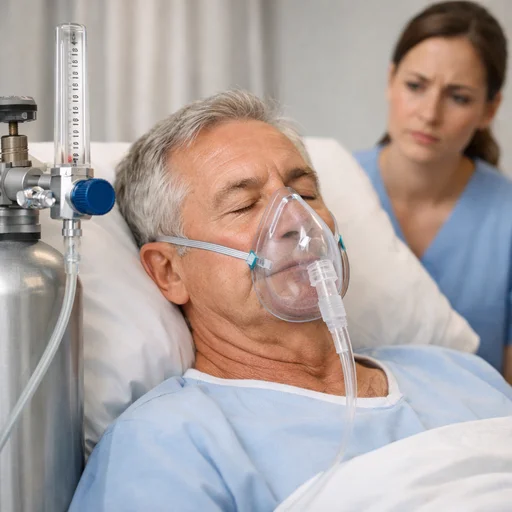
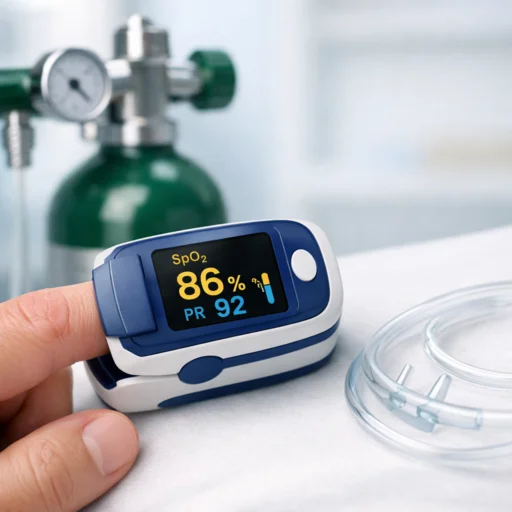
Medical oxygen therapy is genuinely life-saving. It helps people with COPD, pneumonia, heart failure, and severe asthma breathe when their bodies can’t manage on their own. A pulse oximeter clipped to your finger can confirm your blood oxygen level in seconds, and if that number drops, supplemental oxygen can pull you back from the edge.
But here’s the thing most people don’t realize: oxygen is a drug. It has a dose. Go too low, and you’re in trouble. Go too high… and you’re also in trouble.
The air we breathe every day contains about 21% oxygen. In medical settings, patients can receive concentrations ranging from 21% all the way up to 100%. That’s a massive range. And at the higher end, the body starts struggling with what it’s receiving.
What Is Oxygen Toxicity?
The medical term for what happens when a patient uses too much oxygen is hyperoxia, or oxygen toxicity.
When oxygen levels get too high, the tiny air sacs in the lungs, called alveoli, can fill with fluid or collapse entirely. The lungs then struggle to move oxygen into the blood, which is the opposite of what the therapy was meant to achieve.
Think about that for a moment. The treatment designed to help you breathe can, if overdone, make breathing harder.
Researchers at Gladstone Institutes found that excess oxygen essentially “rusts” proteins inside your cells. Oxygen reacts with iron-sulfur clusters in critical proteins, triggering a cascade that damages cells and tissues throughout the body. It’s an elegant but brutal mechanism.
Two Types of Oxygen Toxicity
Not all oxygen overexposure looks the same. There are two distinct patterns, and they depend on how much oxygen is delivered and for how long.
Acute Oxygen Toxicity (High Dose, Short Time)
When a patient is exposed to very high concentrations of oxygen for a short duration, the result is acute toxicity, which primarily affects the central nervous system.
Symptoms can include tunnel vision, ringing in the ears, nausea, facial twitching, dizziness, and confusion. In serious cases, this progresses to seizures. The convulsions follow three phases: a tonic phase with generalized muscle tension, a clonic phase with active convulsions, and a post-critical phase. The patient typically has no memory of the episode.
This type of toxicity is most common in hyperbaric oxygen therapy or in divers breathing enriched oxygen mixtures at depth.
Chronic Oxygen Toxicity (Lower Dose, Longer Time)
Evidence of declining lung function can appear in as little as 24 hours of continuous exposure to 100% oxygen. Diffuse alveolar damage and the onset of acute respiratory distress syndrome typically appear after 48 hours.
After roughly 12 hours of high-dose oxygen exposure, patients may experience lung congestion, pulmonary edema, and collapse of parts of the lung. The resulting fluid buildup causes shortness of breath combined with a burning sensation in the throat and chest, making breathing painful.
This is the type of toxicity that can affect patients on long-term mechanical ventilation or those using home oxygen equipment at too high a flow rate.
Who Is at Risk?
Those at particular risk for oxygen toxicity include patients undergoing hyperbaric oxygen therapy, patients on prolonged high-level oxygen support, premature infants, and underwater divers.
Premature babies deserve special mention. Preterm newborns are at higher risk for bronchopulmonary dysplasia with extended exposure to high oxygen concentrations, and high oxygen exposure may contribute to a condition called retinopathy of prematurity, which can damage developing eyesight.
COPD patients also face a specific and serious risk. In patients with COPD and similar conditions, too much oxygen can cause carbon dioxide narcosis by suppressing the hypoxemic drive that normally tells the body to keep breathing. Their bodies have adapted to low oxygen levels as their breathing signal. Flood that system with oxygen, and the signal gets confused.
How to Use Oxygen Safely
The solution isn’t to avoid oxygen therapy. It’s to use it correctly, at the prescribed flow rate, for the prescribed duration, with proper monitoring.
Current guidelines for patients on mechanical ventilation recommend keeping inspired oxygen concentration below 60%. Beyond that threshold, the risk of pulmonary damage climbs significantly.
If you’re using an oxygen cylinder or oxygen concentrator at home, always follow your doctor’s prescription for flow rate. More is not better. Precision matters.
A pulse oximeter is a simple, affordable tool that lets you monitor your blood oxygen saturation in real time. Most doctors recommend keeping levels between 94% and 98% for most patients, though targets can vary depending on the condition being treated. If you’re consistently above 99% on supplemental oxygen, that’s worth a conversation with your physician.
So, What Does this Mean?
Oxygen is not a supplement you can take freely and assume more is better. It’s a medical gas with real therapeutic windows and real risks when those windows are ignored.
Most patients do recover from oxygen toxicity, especially when it’s caught early. The best prevention is using the lowest effective oxygen concentration for your condition.
If you’re managing oxygen therapy at home, work closely with your healthcare provider. Use the right equipment, at the right settings. And if something feels off, including chest tightness, unusual dizziness, or worsening breathing, don’t wait. Get checked.
At Marium Oxygen, our delivery team helps with installation and setup so that patients and families in Dhaka aren’t left guessing about how to use their equipment. Getting the dose right starts with getting the setup right.