Your body is quietly doing something remarkable right now. Every few seconds, your lungs pull in air, strip out oxygen, and push it into your bloodstream. Your heart pumps it to every cell in your body. It happens automatically. Effortlessly. Until it doesn’t.
When oxygen levels fall, things go wrong fast. The brain gets foggy. The heart works harder. Organs start struggling. So the question isn’t just academic. It’s one of the most important numbers you or someone you love might ever need to know.
Understanding SpO2: The Number That Matters
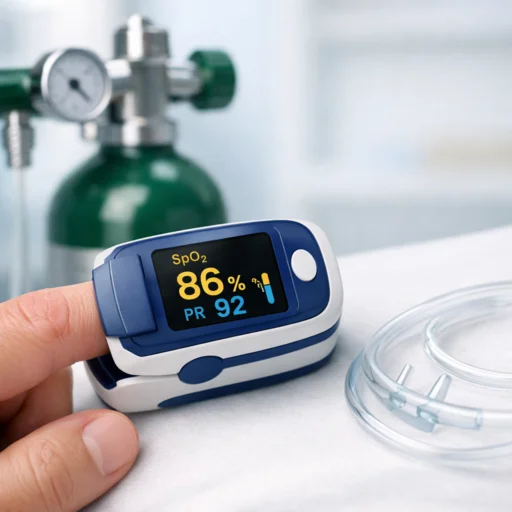
Oxygen saturation, written as SpO2, measures the percentage of your hemoglobin that is carrying oxygen. Normal arterial blood oxygen saturation in healthy people ranges from 96% to 100%. That’s your baseline. That’s what “fine” looks like.
A pulse oximeter measures this through a small clip placed on your finger or toe. It sends infrared light through your skin and reads how much is absorbed by the hemoglobin in your blood. It’s painless. It takes seconds. And it gives you a number that can tell you a lot about what’s going on inside.
When Do You Need Supplemental Oxygen?
Here’s where it gets specific.
Normal SpO2 readings for healthy individuals typically range from 95% to 100%. Readings between 90% and 94% may signal mild hypoxemia. If your SpO2 drops below 90%, medical attention is recommended, as this is considered clinically significant hypoxemia, and supplemental oxygen is often prescribed at this point.
Below 90% is the threshold most clinicians watch closely. Arterial blood oxygen levels below 80% may compromise organ function, including the brain and heart, and should be addressed without delay. Continued low oxygen levels may lead to respiratory or cardiac arrest.
That’s not a gradual decline you can sit with. That’s a medical situation.
The Exception: Chronic Lung Conditions Like COPD
Not everyone’s “normal” looks the same. This is something people often get wrong.
For patients with chronic respiratory conditions like COPD, the target SpO2 range is often lower, between 88% and 92%. For someone without any lung disease, 89% would be alarming. For a long-term COPD patient, it might be their everyday baseline. Giving them too much supplemental oxygen too fast can actually cause problems. The body of someone with chronic hypercapnic respiratory failure has adapted to running on lower oxygen, and flooding it with high-flow O2 can suppress their drive to breathe.
So the rule isn’t just “below 90%, give oxygen.” It’s “below 90% for most people, and know your patient.”
Symptoms That Tell You Something Is Wrong
Numbers matter. But so does how someone looks and feels.
When the brain doesn’t receive enough oxygen, a patient can become confused, lethargic, and eventually fall into a coma. When muscles are deprived of oxygen, they begin to ache. The body tries to compensate by increasing both breathing rate and heart rate.
Watch for those signs. Rapid breathing, confusion, bluish lips or fingertips, and a racing heart are all signs that the body is struggling to keep up. Don’t wait for the number to fall further. Trust what you see.
How Medical Oxygen Is Delivered
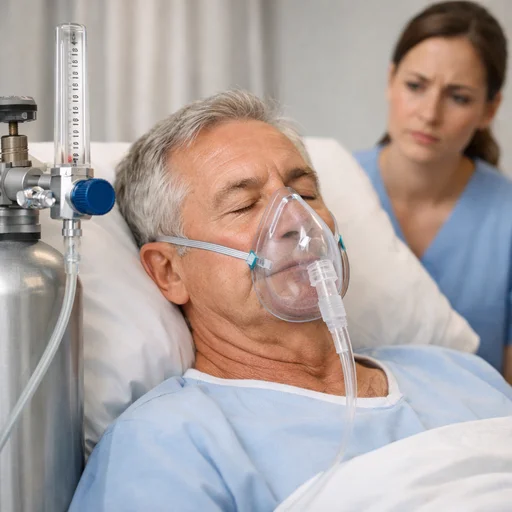
Once a doctor determines that supplemental oxygen is needed, delivery methods vary based on severity.
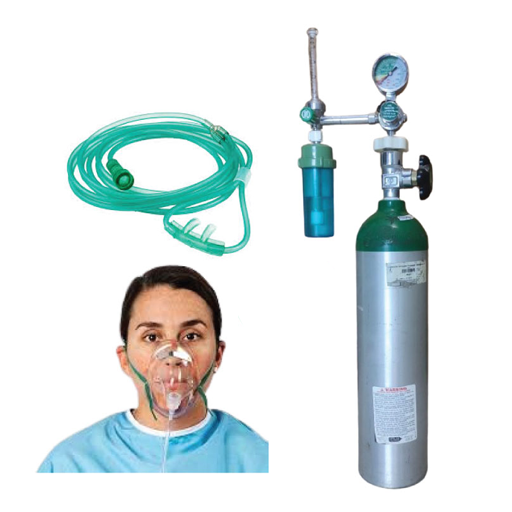
Mild cases often use nasal cannulas, which are the thin tubes that sit under the nostrils. More severe drops in SpO2 may require a simple face mask or a high-flow system. In acute emergencies, a non-rebreather mask at high flow delivers near-pure oxygen to the patient.
At home, people with chronic conditions often use an oxygen concentrator, which pulls oxygen from the surrounding air rather than relying on stored tanks. For emergencies or where a continuous supply is critical, an oxygen cylinder is often the faster, more reliable option.
Knowing which to use, and when, can make a real difference.
Monitoring at Home: Why a Pulse Oximeter Is Worth Having
If someone in your household has a respiratory condition, asthma, heart disease, or even recovered from a severe illness, keeping a pulse oximeter at home is a practical decision. It’s a small, easy-to-use device that gives you real-time data to help you act quickly when it counts.
If your SpO2 level falls below 92%, a doctor may recommend an arterial blood gas test for a more precise reading. A home reading below that range is a signal to call someone. Don’t dismiss it.
When to Seek Help Immediately
To summarize it simply:
95–100% — Normal. No action needed. 90–94% — Watch closely. Consult a doctor, especially if symptomatic. Below 90% — Seek medical attention. Supplemental oxygen is likely needed. Below 80% — Emergency. Organ function is at risk.
These thresholds apply to most healthy adults. Anyone with an existing lung or heart condition should follow the specific targets set by their doctor.
Final Thought
Oxygen saturation is one of the clearest, most immediate indicators of respiratory health. The number tells you when the body is struggling to keep up, often before symptoms become obvious. Understanding what the thresholds mean and having the tools to monitor them puts you in a much better position to respond quickly when it matters.
If you are in Bangladesh and need a reliable oxygen supply at home or for a loved one, Marium Oxygen provides government-approved medical oxygen with 24/7 support and delivery within 60 minutes inside Dhaka city. Whether you need to rent, buy, or refill, having a trusted source already lined up before an emergency is always the smarter move.