When someone you care about receives a cystic fibrosis diagnosis, the questions start piling up fast. Will they need oxygen? When? And what does that mean for their daily life?
The answer isn’t straightforward. Not everyone with cystic fibrosis needs supplemental oxygen, but many do at some point, especially as the condition progresses. Understanding when and why oxygen becomes necessary can help you prepare and advocate for better care.
What Cystic Fibrosis Does to the Lungs
Cystic fibrosis creates thick, sticky mucus that clogs the airways. This isn’t just uncomfortable. It blocks air from reaching the tiny air sacs in the lungs where oxygen enters the bloodstream and carbon dioxide gets expelled. Over time, these mucus plugs cause infections and inflammation that damage lung tissue permanently.
As lung function declines, the body struggles to maintain normal oxygen levels. The medical term for low blood oxygen is hypoxemia. When oxygen saturation drops below what the body needs, organs and tissues can’t function properly.
When Do People with Cystic Fibrosis Need Oxygen?
Here’s where it gets personal. Some children with CF rarely need oxygen. Others might need it during sleep or exercise long before they need it during the day.
Children with cystic fibrosis don’t usually need long-term oxygen therapy early in the disease. But oxygen levels typically drop first during sleep or physical activity before becoming low during waking hours.
Doctors watch for specific signs. They measure oxygen saturation using a device called a pulse oximeter. Medical teams typically start oxygen therapy when overnight oxygen saturation averages 93% or below, or when daytime levels fall to 95% or less.
The symptoms that accompany low oxygen can be subtle at first. People with CF and low oxygen levels may experience reduced ability to exercise, weaker muscles, poor sleep quality, and diminished quality of life. Some notice they’re more tired than usual or can’t keep up with activities they used to manage easily.
Different Types of Oxygen Therapy
Not all oxygen therapy looks the same. Some people need it continuously, while others only use it at night or during physical activity. The delivery method matters too.
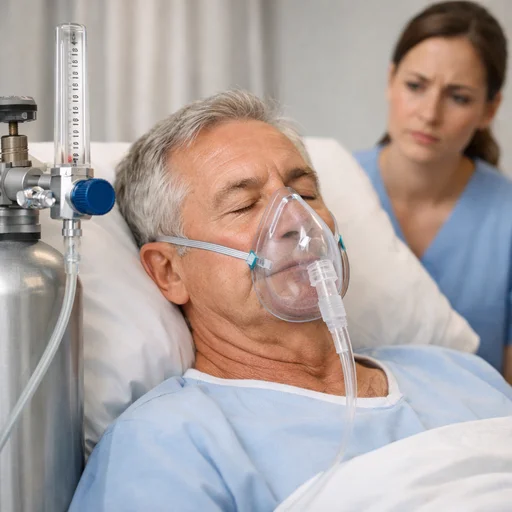
Standard oxygen therapy uses nasal cannulas connected to an oxygen concentrator or oxygen cylinder. Portable units give people freedom to move around and maintain their routines. For those who need oxygen support at home, having reliable equipment makes all the difference.
High-flow oxygen therapy represents a newer approach. Studies show high-flow oxygen therapy can improve comfort and respiratory rate compared to standard oxygen delivery in cystic fibrosis patients.
Does Oxygen Therapy Actually Help?
This is where the evidence gets complicated. Short-term studies show oxygen therapy improves blood oxygen levels in people with CF during sleep and exercise, though it also increases carbon dioxide levels.
People receiving low-flow oxygen could exercise longer and showed more regular attendance at school or work. That’s significant when you’re trying to maintain normalcy while managing a chronic condition.
But the long-term picture remains less clear. Research suggests that nighttime oxygen treatment in cystic fibrosis patients doesn’t appear to reduce death rates or hospitalizations. This doesn’t mean oxygen therapy lacks value. It means the decision to start oxygen should focus on symptom relief and quality of life rather than assuming it will change the disease’s overall course.
The Practical Side of Oxygen Use
Living with oxygen therapy changes things. Equipment needs maintenance. Cylinders need refilling. Travel requires planning. These aren’t minor inconveniences when you’re already managing a complex medical condition.
Having access to reliable oxygen supply matters enormously. In Bangladesh, for instance, facilities like Marium Oxygen provide round-the-clock support for patients who need oxygen at home. Quick delivery and refill services mean you’re not left scrambling during an emergency.
The financial side can’t be ignored either. Oxygen therapy equipment and supplies represent ongoing costs. Understanding your options for purchasing, renting, or refilling cylinders helps you plan ahead.
What About Disease Progression?
Here’s something many people don’t realize: FEV1, which measures how much air you can forcefully exhale in one second, serves as the prime indicator for disability and predicts survival length. As this number drops, oxygen needs typically increase.
Chronic and recurrent respiratory infections damage the lungs progressively, eventually leading to chronic low oxygen levels. This progression happens at different rates for different people. Some maintain good lung function for years. Others see more rapid decline.
The key is monitoring. Regular lung function tests catch problems early. Overnight oxygen studies reveal drops in saturation that happen during sleep. Exercise testing shows how the body responds to physical stress.
Making the Decision About Oxygen
Doctors look at several factors when recommending oxygen therapy. Blood oxygen levels matter most, but symptoms count too. If someone feels constantly exhausted or struggles with daily activities despite acceptable oxygen numbers, supplemental oxygen might still help.
The decision also considers quality of life. If oxygen therapy means better sleep, more energy, and the ability to stay active longer, those benefits matter. The goal isn’t just extending life but making the life you have feel worth living.
Supporting Someone Who Needs Oxygen
If your loved one with cystic fibrosis needs to start oxygen therapy, your support makes a difference. Learning how to operate the equipment takes pressure off them. Understanding when to call for medical help prevents small problems from becoming emergencies.
Keep equipment clean and well-maintained. Monitor oxygen levels with a pulse oximeter if recommended by the medical team. Stay alert for signs that oxygen needs are changing, like increased fatigue or shortness of breath.
The reality is
Do people with cystic fibrosis need medical oxygen? Sometimes, yes. As the disease progresses and lung function declines, many people with CF eventually need supplemental oxygen during sleep, exercise, or continuously throughout the day.
The timing varies tremendously. Some people need oxygen relatively early in their disease course. Others maintain adequate oxygen levels for decades. What matters is proper monitoring and timely intervention when oxygen levels drop.
Oxygen therapy can improve exercise capacity, sleep quality, and daily functioning. While evidence for long-term survival benefits remains limited, the impact on quality of life shouldn’t be underestimated. When breathing becomes harder and oxygen levels fall, supplemental oxygen helps people with cystic fibrosis stay active and engaged with life.
If you or someone you love has cystic fibrosis, talk with your medical team about oxygen monitoring. Early awareness of declining oxygen levels allows for better planning and smoother transitions when therapy becomes necessary. Having reliable access to oxygen equipment and support services means one less thing to worry about when managing this complex condition.